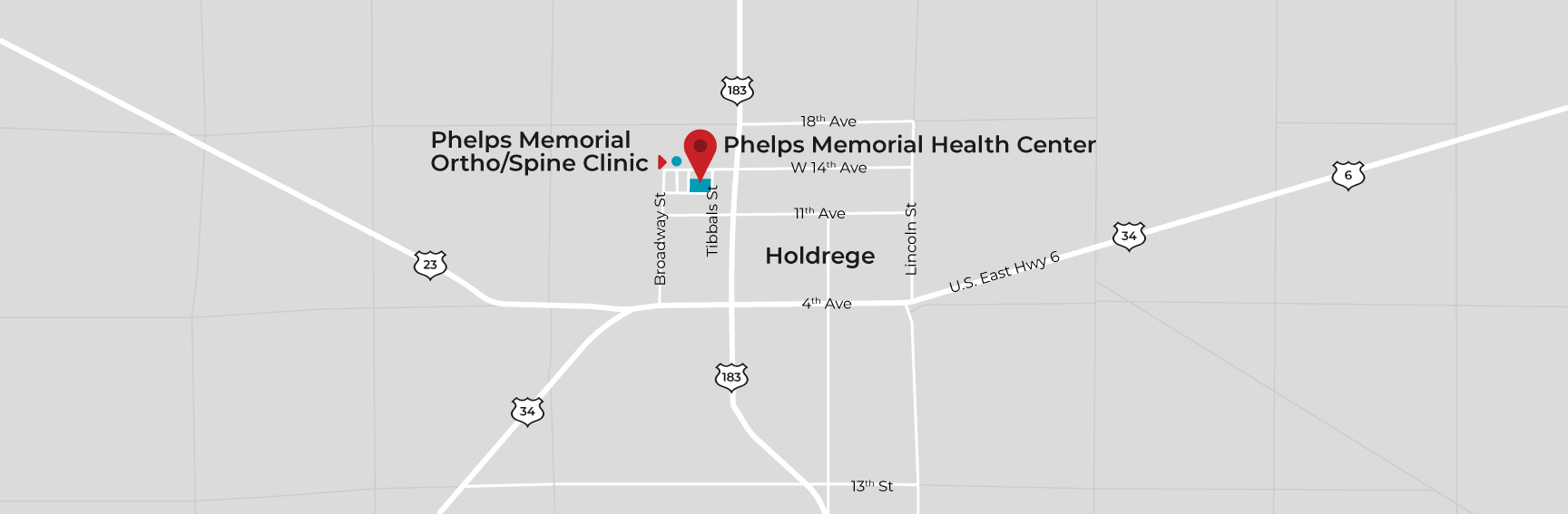
Phelps Memorial Health Center is dedicated to meeting the healthcare needs of our community by providing excellent care. For details about our current visitor policy or treatment and testing of coronavirus, please see the information below.
For more information on the virus itself, or guidelines to follow for prevention and isolation, please visit this CDC website at https://www.cdc.gov/coronavirus/2019-ncov/index.html
Can I get tested at PMHC?
If you are sick enough to need emergent care, you can be tested in our emergency department. Otherwise, our local clinics offer testing by appointment only. Please refer to the below locations and set up your appointment accordingly.
As a reminder, if you are experiencing persistent chest pain or pressure, new confusion, or trouble breathing, please seek emergency medical care.
Phelps Medical Group
Appointment may be required
308-995-6111
Family Medical Specialties
Appointment may be required
308-995-4431
Holdrege VA Clinic
Appointment may be required
308-995-3760
Two Rivers Health Department
Check calendar for dates/locations
https://www.trphd.org/covid-19/event-calendar.html
Walgreens (Kearney, Hastings, North Platte)
https://www.walgreens.com/findcare/covid19/testing?ban=covidfy21_newtestingpg_heroban
To order free at-home COVID tests, visit the COVIDtests.gov website.
Can I visit PMHC?
Visitor Guidelines - updated October 5, 2022
- Visiting hours 7:00 am to 8:00 pm
- Visitors must be healthy to visit
- Each visitor will be screened daily by the front admission team for:
- Positive COVID-19 test in the last 10 days
- Symptoms of COVID-19 (fever or chills, cough, shortness of breath or difficulty breathing, fatigue, muscle or body aches, headache, new loss of taste or smell, sore throat, congestion or runny nose, nausea or vomiting, diarrhea)
- Temperature—if the temperature is 100.0 or above you will not be permitted to visit that day.
- The team will give you a sticker to wear following the screening to notify team members you have had a daily screening performed.
- All visitors who have no issues identified by screening questions will be allowed to enter the facility with NO mask necessary. If you do not pass the screening questions, you will be asked to wear a mask before entering the facility.
- Children are permitted to visit and follow above guidelines as well.
- All visitors are expected to practice social distancing (6 feet) while in the facility
If these guidelines are unable to be followed, you will be asked to not continue visitation.
What should I do if I'm experiencing COVID-19 symptoms?
If you are experiencing symptoms, it's best to call ahead and discuss this with your local health care provider. We can then further advise if you're safe to monitor at home or if you should be seen in the clinic, the ER, or by virtual appointment.
Symptoms you should be monitoring for are fever, cough, shortness of breath, and/or sore throat. A fever is defined at 100.4 degrees. Particularly if you’re working in the health care industry, we want to know if you have a temp of 100.0 or higher. Please check your temperature if you think you may have been exposed to COVID or are experiencing symptoms.
Wash Your Hands
#WashYourHands #InThisTogether #PreventTheSpread